
Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. New York, NY: McGraw-Hill 2011. Accessed October 16, 2014. Qureshi N, Al-Mogbil M, Kentab OY. Hypoglycemia and Metabolic Emergencies in Infants and Children. In: Tintinalli JE, Stapczynski J, Ma O, Cline DM, Cydulka RK, Meckler GD, T. eds. Recommendations are nicely summarized in the table below: Patient AgeĦ mL/kg/h D10 for the first 10 kg + 3 mL/kg/h for 11–20 kg + 1.5 mL/kg/h for each additional kg >20 kg In adolescents and adults the dose is 1ml/kg of D50 (we usually give 2 amps) In these patients it has been shown to reduce rebound hypoglycemia due to endogenous insulin release in response to hyperglycemia from a larger bolus of glucose. Volume start at goal for adults/pediatrics based on fluid balance of patient Neonates usually start lower and advance to goal Amino acids start at goal Dextrose start low and go slow Dependent on glucose infusion rate (GIR) IVFE start at 1 g/kg/day and advance to goal A.S.P.E.N. Of note, it is sometimes recommended to give 0.2ml/kg of D10 as a bolus prior to infusion for neonates. The electrolyte content of intravenous maintenance fluid for infants and children with normal serum electrolyte levels should be 5 percent dextrose and 25 percent normal saline, plus 20 mEq per L. Practically speaking this translates into 5ml/kg of D10 for newborns, and 2ml/kg of D25 for infants and children. Now, this child also has a 5 fluid deficit. 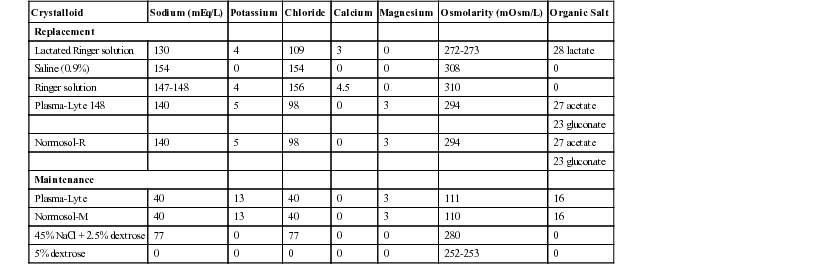
The total amount of sodium to be administered in that maintenance fluid is 44 mEq. One uses normal saline containing approximately 35 mEq/l, and from our calculation, one needs 1250 cc’s of fluid per 24 hours. Repletion fluid therapy corrects water and acute electrolyte deficits that have accrued via. The maintenance volume is calculated using the standard formula. Both 0.2 NaCl and 0.45 NaCl are hypotonic fluids, 0. Most physicians have been taught to use 0.9 NaCl (normal saline) for boluses, and either dextrose 5 with 0.2 NaCl (D5 quarter-normal) or dextrose 5 with 0.45 NaCl (D5 half-normal) for maintenance. IV dextrose is the primary treatment, at a dose of 0.5-1 mg/kg Maintenance requirements vary depending on the patient's underlying clinical status and setting, especially in postoperative or hospitalized children, due to changes in their physiologic responses (eg, excess antidiuretic hormone ADH secretion). This was WB Schwartz and colleagues’ first description of SIADH. A 3 year old M presents to the ED with lethargy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
